Intestinal Microbiome
'Normal' Bacteria Vital for Keeping Intestinal Lining Intact
August 1, 2014 — (BRONX, NY) — Scientists at Albert Einstein College of Medicine of Yeshiva University have found that bacteria that aid in digestion help keep the intestinal lining intact. The findings, reported online in the journal Immunity, could yield new therapies for inflammatory bowel disease (IBD) and a wide range of other disorders.

Sridhar Mani, M.D.The research involved the intestinal microbiome, which contains some 100 trillion bacteria. The role of these microorganisms in promoting or preventing disease is a major emerging field of study. Einstein scientists found that absorption of a specific bacterial byproduct is crucial for maintaining the integrity of the intestinal epithelium—the single-cell layer responsible for keeping intestinal bacteria and their toxins inside the gut and away from the rest of the body. Breaching of the intact intestinal epithelium is associated with a number of diseases.
“Intestinal bacteria secrete a wide variety of chemicals known as metabolites,” said Sridhar Mani, M.D., co-corresponding author of the paper. “These bacteria and their metabolites were known to influence the intestinal epithelium’s integrity, but precisely how they did so wasn’t known.” Dr. Mani is professor of medicine and of genetics and the MiriamMandel Faculty Scholar in Cancer Research at Einstein and attending physician, oncology at the Montefiore Einstein Center for Cancer Care and Montefiore Medical Center.
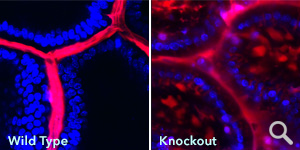
Snapshot images show intestines of wild-type and knockout mice injected with …Dr. Mani and his colleagues suspected that bacterial metabolites exert their influence by binding to and activating a protein in the nuclei of intestinal epithelial cells called the pregnane X receptor (PXR). PXR was known to be activated by chemicals within the body (such as bile acids) as well as by drugs including steroids and antibiotics.
In a series of mouse studies, the researchers found that a metabolite called indole 3-propionic acid (IPA)—produced exclusively by so-called commensal bacteria, which aid in digestion—both strengthens the intestinal epithelium’s barrier function and prevents its inflammation by activating PXR. More specifically, PXR activation suppresses production of an inflammatory protein called tumor necrosis factor alpha (TNF-α) while increasing levels of a protein that strengthens the junctions between adjacent intestinal epithelial cells.
“By adding probiotics in the form of IPA-producing bacteria to the intestine or by administering IPA directly, we may be able to prevent or treat IBD and other inflammatory disorders that occur when the intestinal epithelium has been compromised,” said Dr. Mani. “Such a strategy could also be tried for other health problems that may occur when the intestinal epithelium breaks down, including certain forms of liver disease, diabetes, asthma, allergies, obesity and heart disease.”
Dr. Mani’s team is now developing novel probiotics aimed at restoring the intestinal epithelium’s barrier function by encouraging IPA’s interaction with PXR.
“By adding probiotics…we may be able to prevent or treat IBD and other inflammatory disorders that occur when the intestinal epithelium has been compromised.”
– Sridhar Mani, M.D.
The paper, titled “Symbiotic Bacterial Metabolites Regulate Gastrointestinal Barrier Function via the Xenobiotic Sensor PXR and Toll-like Receptor 4,” was published online in Immunity on July 24, 2014. Other Einstein authors are Madhukumar Venkatesh, Ph.D, Subhajit Mukherjee, M.S., Hongwei Wang, Ph.D., and Hao Li, Ph.D. Other co-authors included Katherine Sun, M.D., Ph.D., at Einstein and Montefiore, Matthew Redinbo, Ph.D., at University of North Carolina at Chapel Hill, Robert Phillips, Ph.D., at University of Georgia, James Fleet, Ph.D., at Purdue University, Sandhya Kortagere, Ph.D., at Drexel University College of Medicine, Alessio Fasano, M.D., at MassGeneral Hospital for Children, Marc Dumas, Ph.D., Jessica Le Ven Ph.D., Pharm D, Jeremy Nicholson, Ph.D., all at Imperial College London, and Alaxandre Bénéchet, M.S, Zhijuan Qiu, M.S, Leigh Maher, M.S., and co-corresponding author Kamal Khanna, Ph.D., all at University of Connecticut Health Center.
The research was supported by National Institutes of Health grants CA127231, CA161879 and Damon Runyon Foundation Clinical Investigator Award (CI 1502) P30CA013330. The authors report no conflicts of interest.
Other Top Stories
9/11 World Trade Center Exposure Linked to Heart Disease Among NYC Firefighters
On Becoming a Physician: New Einstein Students Receive White Coats and Stethoscopes
Novel Therapy for Acute Migraine Shows Promise in Phase 3 Clinical Trial
First Complete Wiring Diagram of an Animal's Nervous System
Multimillion Dollar NIH Grant to Help Reduce Opioid Use & Get Care to People Who Need It
NIH Grant Funds $23 Million Study of Diseases Affecting People Living with HIV
New TAILORx Data Guides Adjuvant Therapy in Younger Breast Cancer Patients
Einstein Celebrates Its 61st Commencement
Bolstering Biopsies: Testing Patients' Individual Cells to Guide Treatment



Tablet Blog